Topic Overview
Is this topic for you?
If you have had a C-section and would like information about how a caesarean affects future deliveries, see the topic Vaginal Birth After Caesarean (VBAC).
What is a caesarean section?
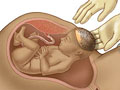
A caesarean section is the delivery of a baby through a cut (incision) in the mother's belly and uterus. It is often called a C-section. In most cases, a woman can be awake during the birth and be with her newborn soon afterward. See a picture of a delivery by C-section.
If you are pregnant, chances are good that you will be able to deliver your baby through the birth canal (vaginal birth). But there are cases when a C-section is needed for the safety of the mother or baby. So even if you plan on a vaginal birth, it's a good idea to learn about C-section, in case the unexpected happens.
When is a C-section needed?
A C-section may be planned or unplanned. In most cases, doctors do caesarean sections because of problems that arise during labour. Reasons you might need an unplanned C-section include:
- Labour is slow and hard or stops completely.
- The baby shows signs of distress, such as a very fast or slow heart rate.
- A problem with the placenta or umbilical cord puts the baby at risk.
- The baby is too big to be delivered vaginally.
When doctors know about a problem ahead of time, they may schedule a C-section. Reasons you might have a planned C-section include:
- The baby is not in a head-down position close to your due date.
- You have a problem such as heart disease that could be made worse by the stress of labour.
- You have an infection that you could pass to the baby during a vaginal birth.
- You are carrying more than one baby (multiple pregnancy).
- You had a C-section before, and you have the same problems this time or your doctor thinks labour might cause your scar to tear (uterine rupture).
In some cases, a woman who had a C-section in the past may be able to deliver her next baby through the birth canal. This is called vaginal birth after caesarean (VBAC). If you have had a previous C-section, ask your doctor if VBAC might be an option this time.
In the past 40 years, the rate of caesarean deliveries has jumped from about 1 out of 20 births to about 1 out of 3 births.footnote 1 This trend has caused experts to worry that C-section is being done more often than it is needed. Because of the risks, experts feel that C-section should only be done for medical reasons.
What are the risks of C-section?
Most mothers and babies do well after C-section. But it is major surgery, so it carries more risk than a normal vaginal delivery. Some possible risks of C-section include:
- Infection of the incision or the uterus.
- Heavy blood loss.
- Blood clots in the mother's legs or lungs.
- Injury to the mother or baby.
- Problems from the anesthesia, such as nausea, vomiting, and severe headache.
- Breathing problems in the baby if it was delivered before its due date.
If she gets pregnant again, a woman with a C-section scar has a small risk of the scar tearing open during labour (uterine rupture). She also has a slightly higher risk of a problem with the placenta, such as placenta previa.
How is a C-section done?
Before a C-section, a needle called an IV is put in one of the mother's veins to give fluids and medicine (if needed) during the surgery. She will then get medicine (either epidural or spinal anesthesia) to numb her belly and legs. Fast-acting general anesthesia, which makes the mother sleep during the surgery, is only used in an emergency.
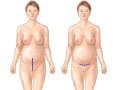
After the anesthesia is working, the doctor makes the incision. Usually it is made low across the belly, just above the pubic hair line. This may be called a "bikini cut." Sometimes the incision is made from the navel down to the pubic area. See a picture of C-section incisions. After lifting the baby out, the doctor removes the placenta and closes the incision with stitches.
How long does it take to recover from a C-section?
Most women go home 3 to 5 days after a C-section, but it may take 4 weeks or longer to fully recover. By contrast, women who deliver vaginally usually go home in a day or two and are back to their normal activities in 1 to 2 weeks.
Before you go home, a nurse will tell you how to care for the incision, what to expect during recovery, and when to call the doctor. In general, if you have a C-section:
- You will need to take it easy while the incision heals. Avoid heavy lifting, intense exercise, and sit-ups. Ask family members or friends for help with housework, cooking, and shopping.
- You will have pain in your lower belly and may need pain medicine for 1 to 2 weeks.
- You can expect some vaginal bleeding for several weeks. (Use sanitary pads, not tampons.)
Call your doctor if you have any problems or signs of infection, such as a fever or red streaks or pus from your incision.
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
How a Caesarean Section Is Done
Surgery preparation
Most caesarean sections are done with epidural or spinal anesthesia, used to numb sensation in the abdominal area. Only in an emergency situation or when an epidural or spinal anesthesia cannot be used or is a problem would fast-acting general anesthesia be used to make you unconscious for a caesarean birth.
The hospital may send you instructions on how to get ready for your surgery, or a nurse may call you with instructions before your surgery.
In preparation for a caesarean section, your arms are secured to the table for your safety, and a curtain is hung across your chest. A tiny intravenous (IV) tube is placed in your arm or hand; you may be given a sedative through the IV to help you relax. A catheter is inserted into your bladder to allow you to pass urine during and after the surgery. Your upper pubic area may be shaved, and the abdomen and pubic area are washed with an antibacterial solution. The incision site may be covered with an adhesive plastic sheet, or drape, to protect the surgical area.
Before, during, and after a caesarean section, your blood pressure, heart rate, heart rhythm, and blood oxygen level are closely monitored. You will also be given a dose of antibiotics to prevent infection after delivery.
Caesarean procedure and delivery
After the anesthesia is working, a doctor makes the caesarean incision through your lower abdomen and uterus. See a picture of caesarean section incisions. You may notice an intense feeling of pressure or pulling as the baby is delivered. After delivering your newborn through the incision, the doctor then removes the placenta and then closes the uterus and the incision with layers of stitches.
Right after surgery, you will be taken to a recovery area where nurses will care for and observe you. You will stay in the recovery area for 1 to 4 hours, and then you will be moved to a hospital room. In addition to any special instructions from your doctor, your nurse will explain information to help you in your recovery.
Who To See
A caesarean section can be done by a doctor who has specialized training, such as:
- An obstetrician.
- A perinatologist (maternal-fetal medicine specialist).
- A family doctor with caesarean section training.
- A surgeon.
If your pregnancy care provider doesn't perform caesareans and foresees a possible need for a caesarean, you will be referred to a caesarean-trained doctor ahead of time. Your family medicine doctor or registered midwife can assist with the surgery and provide your follow-up care.
Why It Is Done
Some caesarean deliveries are planned ahead of time. Others are done when a quick delivery is needed to ensure the mother's and infant's well-being.
Planned caesarean
Some caesarean sections are planned when a known medical problem would make labour dangerous for the mother or baby. Medical reasons for a planned caesarean may include:
- A fetus in any position that is not head-down (including breech position). For more information, see the topic Breech Position and Breech Birth.
- Decreased blood supply to the placenta before birth, which may lead to a small baby.
- Your baby is thought to be very large.
- A maternal disease or condition that may be made worse by the stress of labour. One example is heart disease.
- A known health problem with the baby, such as spina bifida.
- A placenta that is blocking the cervix (placenta previa). For more information, see the topic Placenta Previa.
- Open sores from active genital herpes near the due date, which can be passed to the fetus during vaginal delivery.
- Some cases of human immunodeficiency virus (HIV), which can be passed to the fetus during vaginal delivery.footnote 2
- Multiple pregnancy. The direction and size of the incision depends on the position of the babies. A caesarean section (C-section) may be needed, depending on the position and number of babies, whether they share an amniotic sac, or if you or the babies have any health problems.
Many caesarean deliveries are planned ahead of time for women who have had a caesarean in the past. Reasons for a planned repeat caesarean may include:
- Deciding not to try vaginal birth after caesarean (VBAC) after discussing the risks and benefits with your doctor.
- Factors that increase the risk of uterine rupture during labour, such as having a vertical scar, triplets or more, or a baby thought to be very large. For more information, see the topic Vaginal Birth After Caesarean (VBAC).
- No access to constant medical supervision by a caesarean-trained doctor during active labour, or no available facilities for an emergency caesarean.
Depending on the reason for a planned C-section and the risks to you or your baby, the C-section may be scheduled near your due date or weeks before. Talk to your doctor to learn about the timing that is best for your situation.
Some women request to have a C-section even though they have never had one before and there is no medical need for it. This is called an elective primary C-section. Because of the risks of C-section, experts recommend that C-sections generally be done only for medical reasons. If you're thinking of having a C-section for personal reasons, talk to your doctor as soon as possible about reasons for and against an elective primary C-section.
Unplanned caesarean
Some unplanned caesareans happen when there is a problem before or during labour. Sometimes this is an emergency. Medical reasons for an unplanned caesarean may include:
- Fetal distress (suggested by a very rapid or very slow heart rate).
- Abruptio placenta, which can cause excessive bleeding (hemorrhage) and decreased oxygen supply to the fetus. For more information, see the topic Abruptio Placenta.
- Umbilical cord problems that decrease or cut off fetal blood supply, as when the cord has slipped into the birth canal ahead of the fetus, and the fetus moves into the birth canal and presses against the cord (cord prolapse).
- Difficult, slow labour.
- Labour that has stopped completely.
Risks and Complications
Caesarean section is considered relatively safe. But it does pose a higher risk of some complications than does a vaginal delivery. If you have a caesarean section, expect a longer recovery time than you would have after a vaginal delivery.
After caesarean section, the most common complications for the mother are:
- Infection.
- Heavy blood loss.
- A blood clot in the legs or lungs.
- Nausea, vomiting, and severe headache after the delivery (related to anesthesia and the abdominal procedure).
- Bowel problems, such as constipation or when the intestines stop moving waste material normally (ileus).
- Injury to another organ (such as the bladder). This can occur during surgery.
- Maternal death (very rare). About 2 in 100,000 cesareans result in maternal death.footnote 1
Caesarean risks for the infant include:
- Injury during the delivery.
- Need for special care in the neonatal intensive care unit (NICU).footnote 6
- Immature lungs and breathing problems, if the due date has been miscalculated or the infant is delivered before 39 weeks of gestation.footnote 6, footnote 7
While most women recover from both caesarean and vaginal births without complications, it takes more time and special care to heal from caesarean section, which is a major surgery. Women who have a caesarean section without complications spend about 3 days in the hospital, compared with about 2 days for women who deliver vaginally. Full recovery after a caesarean delivery takes 4 to 6 weeks. Full recovery after a vaginal delivery takes about 1 to 2 weeks.
Long-term risks of caesarean section
Women who have a uterine caesarean scar have slightly higher long-term risks. These risks, which increase with each additional caesarean delivery, include:footnote 8
- Breaking open of the incision scar during a later pregnancy or labour (uterine rupture). For more information, see the topic Vaginal Birth After Caesarean (VBAC).
- Placenta previa, the growth of the placenta low in the uterus, blocking the cervix.
- Placenta accreta, placenta increta, placenta percreta (least to most severe). These problems occur when the placenta grows deeper into the uterine wall than normal, which can lead to severe bleeding after childbirth, and sometimes may require a hysterectomy.
What to Expect After C-Section
After a routine caesarean section, expect to be monitored closely for the next 24 hours to make sure that you don't develop any problems. You will receive pain medicine and will likely be encouraged to begin walking short distances within 24 hours of surgery. Walking can help relieve gas buildup in the abdomen. It is usually very uncomfortable to begin walking, but the pain will decrease in the days after the delivery.
The typical hospital stay after a caesarean delivery is about 3 days. You can feed and care for your newborn as you feel able. Before going home, you'll receive post-surgery instructions, including warning signs of complications. It can take 4 weeks or more for a caesarean incision to heal, and it isn't unusual to have occasional pains in the area during the first year after the surgery.
It is important to take care of yourself at home while you are healing.
Activity
- Rest when you feel tired. Getting enough sleep will help you recover.
- Try to walk each day. Start by walking a little more than you did the day before. Bit by bit, increase the amount you walk. Walking boosts blood flow and helps prevent pneumonia, constipation, and blood clots.
- Avoid strenuous activities, such as bicycle riding, jogging, weightlifting, and aerobic exercise, for 6 weeks or until your doctor says it is okay.
- Until your doctor says it is okay, do not lift anything heavier than your baby.
- Do not do sit-ups or other exercises that strain the belly muscles for 6 weeks or until your doctor says it is okay.
- Hold a pillow over your incision when you cough or take deep breaths. This will support your belly and reduce your pain.
- You may shower as usual. Pat the incision dry when you are done.
- You will have some vaginal bleeding. Wear sanitary pads. Do not douche or use tampons until your doctor says it is okay.
- Ask your doctor when you can drive again.
- You will probably need to take at least 6 weeks off work. It depends on the type of work you do and how you feel.
- Ask your doctor when it is okay for you to have sex.
Diet
- You can eat the foods that are in your normal diet. If your stomach is upset, try bland, low-fat foods like plain rice, broiled chicken, toast, and yogurt.
- Drink plenty of fluids (unless your doctor tells you not to).
- You may notice that your bowel movements are not regular right after your surgery. This is common. Try to avoid constipation and straining with bowel movements. You may want to take a fibre supplement every day. If you have not had a bowel movement after a couple of days, ask your doctor about taking a mild laxative.
Incision care
- If you have strips of tape on the incision, leave the tape on for a week or until it falls off.
- Wash the area daily with warm, soapy water, and pat it dry. Other cleaning products, such as hydrogen peroxide, can make the wound heal more slowly. You may cover the area with a gauze bandage if it weeps or rubs against clothing. Change the bandage every day.
- Keep the area clean and dry.
For information about how a caesarean affects future deliveries, see the topic Vaginal Birth After Cesarean (VBAC).
When to call a doctor
Call 9-1-1 anytime you think you may need emergency care. For example, call if:
- You have thoughts of harming yourself, your baby, or another person.
- You passed out (lost consciousness).
- You have severe trouble breathing.
- You have sudden chest pain and shortness of breath, or you cough up blood.
- You have a seizure.
- You have severe pain in your belly.
Call your doctor, midwife, or nurse advice line now or seek immediate medical care if:
- You have bright red vaginal bleeding that soaks one or more pads each hour for 2 or more hours.
- Your vaginal bleeding seems to be getting heavier or is still bright red 4 days after delivery.
- You pass blood clots larger than the size of a golf ball.
- You have vaginal discharge that smells bad.
- You are sick to your stomach or cannot keep fluids down.
- You have loose stitches, or your incision comes open.
- Your belly feels tender, or full and hard.
- You have signs of infection, such as:
- Increased pain, swelling, warmth, or redness.
- Red streaks leading from the incision.
- Pus draining from the incision.
- Swollen lymph nodes in your neck, armpits, or groin.
- A fever.
- You have signs of a blood clot, such as:
- Pain in your calf, back of the knee, thigh, or groin.
- Redness and swelling in your leg or groin.
- You have signs of pre-eclampsia, such as:
- Sudden swelling of your face, hands, or feet.
- New vision problems (such as dimness, blurring, or seeing spots).
- A severe headache.
- You have trouble passing urine or stool, especially if you have pain or swelling in your lower belly.
- You feel sad, tearful, or hopeless for more than a few days, or you have troubling or dangerous thoughts.
Some women feel shoulder pain for days after a caesarean section. This is referred pain, caused by trauma to the abdominal muscles during the delivery. It goes away on its own during recovery.
Related Information
References
Citations
- Cunningham FG, et al. (2010). Cesarean delivery and peripartum hysterectomy. In Williams Obstetrics, 23rd ed., pp. 544–564. New York: McGraw-Hill.
- American College of Obstetricians and Gynecologists (2000; reaffirmed 2010). Scheduled cesarean delivery and the prevention of vertical transmission of HIV infection. ACOG Committee Opinion No. 234. Washington, DC: American College of Obstetricians and Gynecologists.
- Alsayegh E, et al. (2018). Caesarean delivery on maternal request, No. 361. Journal of Obstetrics and Gynaecology Canada, 40(7): 967–971. DOI: 10.1016/j.jogc.2017.12.009. Accessed December 21, 2018.
- American College of Obstetricians and Gynecologists (2013, reaffirmed 2017). Cesarean delivery on maternal request. ACOG Committee Opinion No. 559. Obstetrics and Gynecology, 121(4): 904–907. DOI: 10.1097/01.AOG.0000428647.67925.d3. Accessed October 16, 2018.
- American College of Obstetricians and Gynecologists (2013, reaffirmed 2017). Medically indicated late-preterm and early-term deliveries. ACOG Committee Opinion No. 560. Obstetrics and Gynecology, 121(4): 908–910. DOI: 10.1097/01.AOG.0000428648.75548.00. Accessed October 16, 2018.
- Kolås T, et al. (2006). Planned cesarean versus planned vaginal delivery at term: Comparison of newborn infant outcomes. American Journal of Obstetrics and Gynecology, 195(6): 1538–43.
- Tita ATN, et al. (2009). Timing of elective repeat cesarean delivery at term and neonatal outcomes. New England Journal of Medicine, 360(2): 111–120.
- Scott JR, Porter TF (2008). Cesarean delivery. In RS Gibbs et al., eds., Danforth's Obstetrics and Gynecology, 10th ed., pp. 491–503. Philadelphia: Lippincott Williams and Wilkins.
Credits
Current as of: November 9, 2022
Author: Healthwise Staff
Medical Review:
Sarah Marshall MD - Family Medicine
Anne C. Poinier MD - Internal Medicine
Kathleen Romito MD - Family Medicine
Adam Husney MD - Family Medicine
Deborah A. Penava BA, MD, FRCSC, MPH - Obstetrics and Gynecology
Current as of: November 9, 2022
Author: Healthwise Staff
Medical Review:Sarah Marshall MD - Family Medicine & Anne C. Poinier MD - Internal Medicine & Kathleen Romito MD - Family Medicine & Adam Husney MD - Family Medicine & Deborah A. Penava BA, MD, FRCSC, MPH - Obstetrics and Gynecology